What’s Driving Health Care Costs? Overtreatment and Unnecessary Testing
The United States has some of the best, elite treatment facilities, medical institutions, and doctors in the world, and yet some of the worst health outcomes despite possessing cutting-edge technology and the best talent.
We spend massive amounts of money, three times the OECD average to be exact, yet have experienced a reduction in life expectancy the last three decades. The United States is, to put it simply, a ball of contradictions that politicians, healthcare advocates, the government, and the private sector have been unable to untangle. Consider just for a moment that we claim 17 of the 20 best hospitals in the world. We have 7 of the top 10 best medical universities in the world. We spend an enormous $3.3 trillion on healthcare, dwarfing any other country. However, health outcomes have remained stagnant at best.
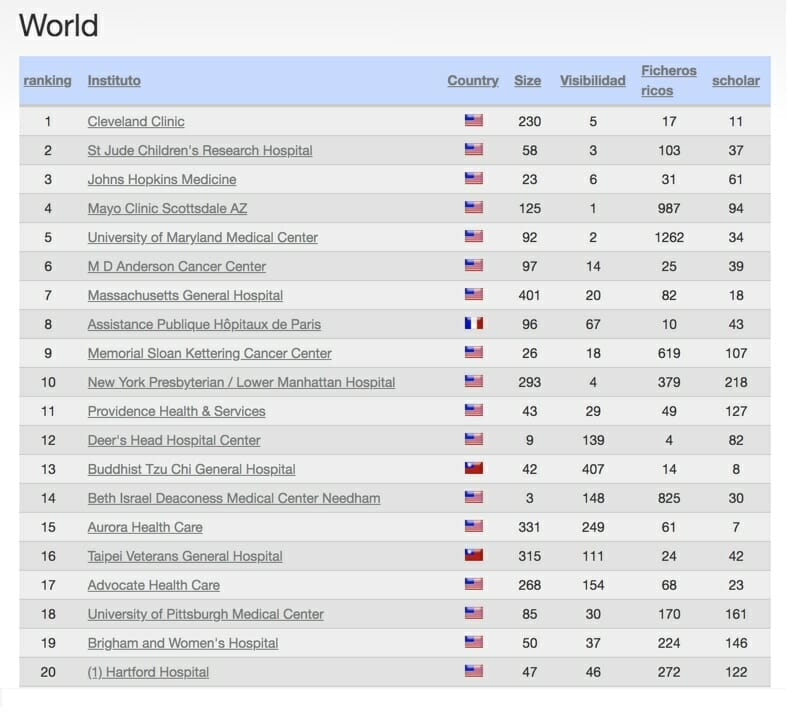
In the context of a healthcare sector distorted by competing interests and warring factions, price opacity, de facto monopolies, and brazen greed and corruption, it comes as little surprise that we are somehow simultaneously the world’s most voracious healthcare consumers and yet one of the least healthy developed nations.
So where does all the extra money go?
There is no simple answer to such a far-reaching question about an industry that constitutes nearly 20 percent of the nation’s GDP. However, there is evidence to suggest that a lot of that money is merely going to waste thanks to human and corporate greed and perverse incentive structures.
The average American spends over $9,000 per year on healthcare. In comparison, the average Swede, the second biggest healthcare spender, only pays around $6,000 per year.
Healthcare Rankings & Expenditures
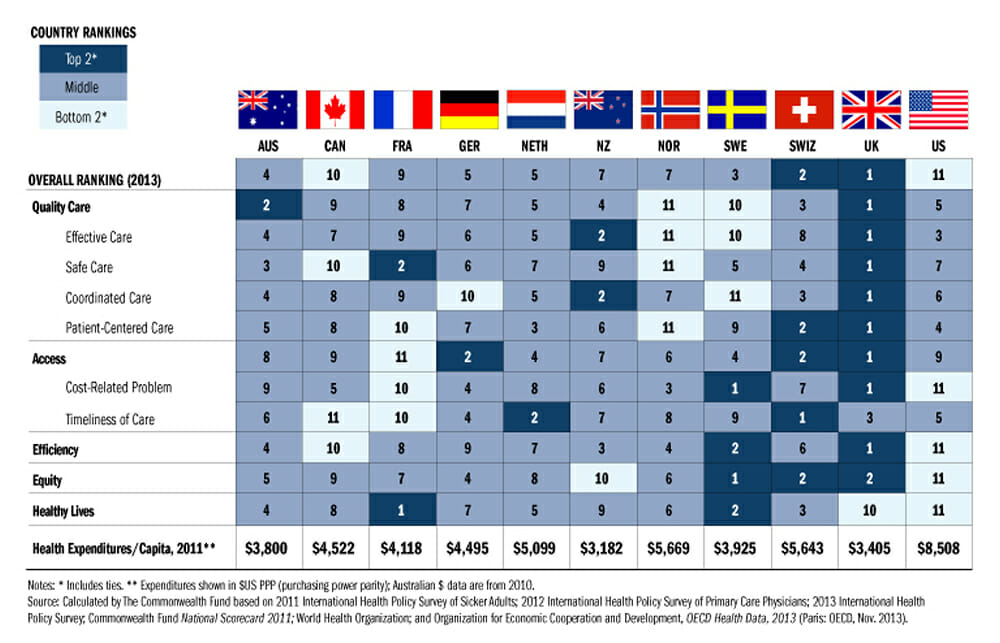
Other OECD nations report even lower levels of personal spending on health care, with the UK spending under $4,000 per person. Even countries such as France and Canada which are notorious for practicing so-called “socialized” medicine spent half as much as the US.
For the amount of money Americans spend on healthcare, we would expect to have the best in the world. However, while we spend twice as much as the average French citizen, our health outcomes lag far behind.
Healthcare Price Inflation
Why is this happening? Why the lopsided relationship between money spent and actual human health?
Some experts blame overtreatment. According to the Institute of Medicine (ICM), unnecessary tests, prescription drugs and medication, and extraneous procedures are one of the drivers of healthcare price inflation.
"The average American spends over $9,000 per year on healthcare. In comparison, the average Swede, the second biggest healthcare spender, only pays around $6,000 per year. "
--- DR. CRISTIN DICKERSON, MD
More Complicated Than Simple “Overutilization”
The systemic underpinnings of our dysfunctional healthcare system are far more prosaic than something as sweeping as unfettered human greed. Yes, 85 percent of doctors admitted calling for too many tests, 97 percent agreed to personally ordering unnecessary tests. However, they did so not necessarily because of greed, but because of a variety of systemic factors that, according to doctors, have forced their hand.
There is a lack of scientific reasoning in the way Americans consume healthcare. Despite little evidence that supplements are needed for a healthy diet except for targeted medical needs, 68% of American adults take dietary supplements. The American Cancer Society says "Exposures to supplements (such as vitamins, herbs, protein powders, and botanicals) accounted for more than 100,000 calls to US poison control centers in 2013. Of these calls, more than 8,000 people were reportedly treated in health care facilities. More than 1000 cases were reported to poison control centers as having moderate to severe outcomes. This did not include electrolyte and mineral supplements, which accounted for another 2,500 people treated in health facilities, with 350 moderate to severe reactions and 2 deaths reported to poison control centers." Additionally, studies like the SELECT trial (Selenium and Vitamin E Cancer Prevention Trial) designed to determine the long-range effect of selenium and vitamin E supplements on development of prostate cancer found a 17 percent increase in the risk of developing prostate cancer in men who took 400 units of vitamin E daily, and no protection against developing prostate cancer from selenium.
Doctors frequently argue that similarly, patients desire testing that is considered medically to be of low value. However, our fee for service reimbursement system does not pay them to take the time to explain the risk-benefit ratio to patients, it is easier just to order the exam.
Doctors also spend on average 7 minutes in a patient encounter. It can be argued that the fee for service model that requires a primary care doctor to see 25 patients a day has doctors substituting imaging and labs for an adequate history and physical.
Doctors also over order to cover legal bases. The United States is notoriously litigious. Doctors often call for a variety of tests, even tests that they might not think are helpful, to ensure that they will not get sued for malpractice down the road. Furthermore, many doctors prefer to err on the side of caution over cost.
Healthcare Problems vs. Healthcare Prevention
Another problem has to do with the way we think about healthcare in this country. In the healthcare system, there is a remarkable focus on directly treating health problems rather than investing in long-term prevention. Doctors and care providers are encouraged and incentivized to attack symptoms when they occur even if that means unnecessarily prescribing medication or running a battery of tests “just to be sure.”
It is the doctor’s duty to pursue treatments and therapies that will benefit the patient. However, a patient’s financial well-being is rarely taken into account. Furthermore, there is no denying that there is a financial incentive to provide more treatment, even if the utility is limited. This industry-wide mindset of finding a cure no matter the cost can lead to extravagant overtreatment and overtesting - often to the detriment of the patient.
Perverse Incentives at Work
According to the Lown Institute, we waste $200 billion per year on unnecessary medical tests. While terrible for healthcare consumers, businesses, and taxpayers footing Medicare and Medicaid bills, that $200 billion has been a massive windfall for industries that sell diagnostic products and services.
It has also been a huge financial win for many hospitals as well as the employed and subsidized doctors that work within and with them, that own and operates testing equipment and services. It only makes sense that when a doctor’s financial interests are aligned with pushing more drugs, or more imaging examinations, or more tests, they may do just that. Add to the fact that 70% of physicians are employed or subsidized by hospitals and the cost of care in those systems is 2 to 3 times higher than the care initiated by an independent doctor.
While there are laws against doctors receiving direct kickbacks, medical testing and imaging is ultimately a referral business. In the case of doctors trying to make an extra buck, self-referrals are a tempting and lucrative way to make a lot more money for the hospital system, increasing their own value to that entity and ultimately what they are paid.
Reintroducing the Free Market: Not What You Might Think
Many people confuse the idea of laissez-faire economics with a truly free and fair market. This is not the case. Under this economic philosophy, there is no intervention to deal with monopolies, unethical middlemen, price opacity, self-dealing, and other real-world factors that might unbalance a classical free market economy.
The US healthcare system is, arguably, suffering from all of these problems.
In the 19th century, this laissez-faire economics was the dominant economic model in the Western world. Soon, however, a disparity in the distribution of wealth, harsh treatment and disregard for safety in the workplace, disregard for consumer safety, and spread of monopolistic entities emerged.
Again, these same issues now plague the US health system.
laissez-faire economics
One of the guiding principles of capitalism, this doctrine claims that an economic system should be free from government intervention or moderation, and be driven only by the market forces. Centered on the belief (termed invisible hand by the 18th-century Scottish economist Adam Smith) that human beings are naturally motivated by self-interest and, when they are not interfered with in their economic activities, a balanced system of production and exchange based on mutual benefit emerges. Laissez-faire (French for, allow to pass or let go) economics originated in the 18th century France where economists (then called 'physiocrats') such as Francois Quesnay (1694-1774) and Victor Riqueti-Marquis de Mirabeau (1715-89) became hostile to subsidies and discriminatory economic measures of then-prevalent mercantilism.
They believed in a bountiful nature and innate goodness of humankind and asserted that governments should leave the individual alone except when social liberties are infringed. In the 19th century, this philosophy became the dominant economic thinking in the Western world. But soon its failings reflected in the great disparity in the distribution of wealth, harsh treatment of workers, disregard for consumer safety, and spread of monopolies, became clear. By the mid 19th century, opposition to laissez-faire economics began and governments in all industrialized countries intervened on behalf of workers and the general population. Factory laws and consumer protection laws were enacted and the growth of monopolies was checked. Early 20th century saw the breakup of monopolies in the US and (after the Second World War) nationalization of essential industries and services in Europe. Keynesian economics (which advocates government intervention in the national economy) further undermined it, a process spurred by the great depression of the 1930s.
From 1970's, however, the pendulum swung back to laissez-faire economics (renamed 'market economy' or 'free enterprise') and brought deregulation of business, and progressive removal of trade barriers, which is continuing.
source: Business Dictionary
Medical monopolies in today’s obstructed markets, for example, can artificially inflate prices for their products because there is no competition. Likewise, hospitals can charge patients whatever they want because there is no price transparency, thereby preventing healthcare consumers from making rational buying decisions. This lack of real competition and transparent information are a major factor in America's inflated healthcare costs.
Overtreatment, overutilization, and medical waste of all kind ultimately stem from incentive structures that have been perverted by a system dominated by factional interests. Until we can somehow truly realign our healthcare system with free market values, overtreatment, and unnecessary testing will always be a feature of the system, not a bug, driving higher healthcare costs.
It is clear our lawmakers whose campaigns are funded by pharmaceutical companies, insurance companies, and hospitals have not and are not going to make necessary changes. However, the employer-sponsored health care market is less encumbered by perverse incentives. In fact, the incentives of employers, individuals, and direct health care providers are beautifully aligned. There is a growing movement to reform employer-sponsored health care by removing the unnecessary middlemen and providing high-quality care at transparent competitive prices. Green Imaging and Lucent MD are proud to be at the forefront of that movement.