Mammogram
Mammograms Save Lives
For women, breast cancer is one of the most common causes of death due to cancer and the cause of unquantifiable suffering.
One-third of all cancers diagnosed in women are breast cancer.
1 in 8 women will develop an invasive form of breast cancer at some point during their lifetimes. In total, a quarter million women will be diagnosed with breast cancer every single year.
Advances In Early Detection
While the specter of being diagnosed with breast cancer remains, advances in early detection, intervention, and improvements in postoperative treatment have significantly decreased mortality and improved the odds of survival.
One of the most important tools in the growing medical arsenal for combatting breast cancer is the humble science of mammography. Women who catch an invasive breast cancer early are likely to survive. The later the detection the lower the odds of survival. Studies show that women 40 years of age and older benefit from regular, either annual or biennial mammograms.
Mammography may be most important in the younger age group as these cancers tend to be more aggressive. Women between the ages of 50 and 59 who undergo regular screenings experience 14 percent lower mortality rates as a group than those who forego it. Similarly, women between 60 and 69 who get mammograms regularly are 33 percent less likely to die from the disease.

What is a Mammogram?
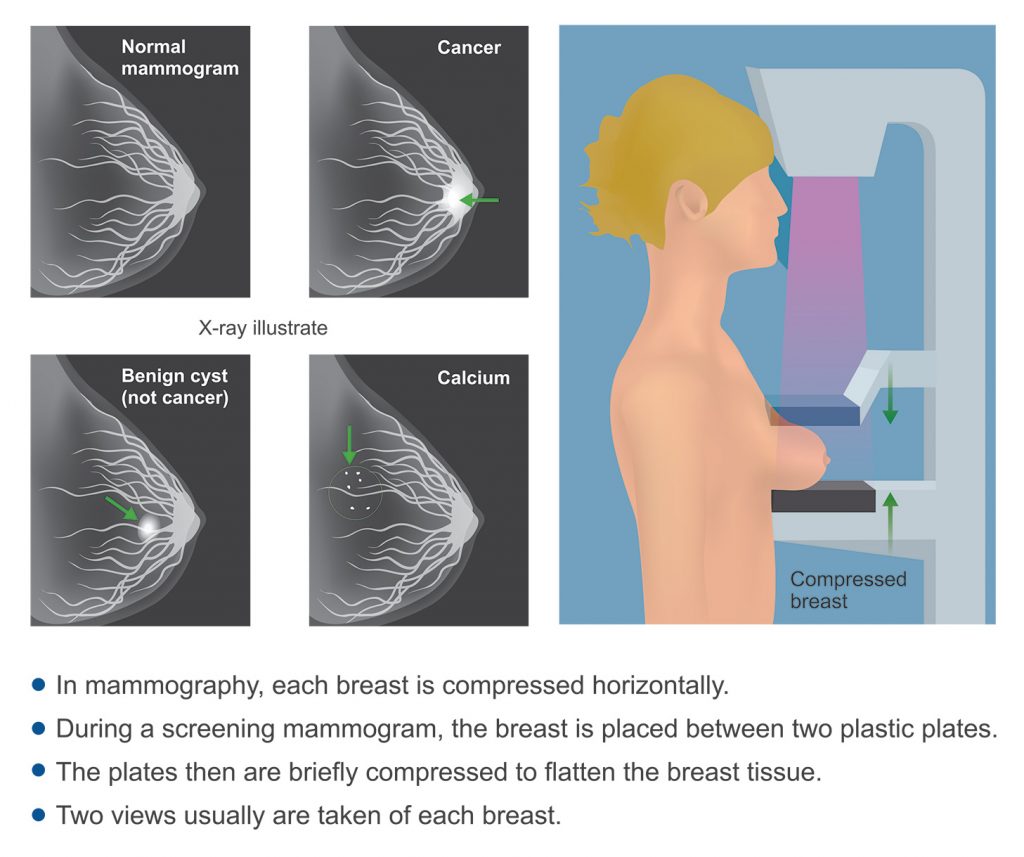
A mammogram is an imaging procedure that most commonly utilizes low-dose x-rays to create a detailed image of the breast, internal anatomical structures, and the existence of any cancerous growths.
The most common use of mammograms by far is for the detection and diagnosis of breast cancer. To this end, there are typically two types of mammograms employed:
- Screening mammograms
- Diagnostic mammograms
Screening Mammograms
Screening mammograms are done in asymptomatic women and typically consist of two images of each breast. Screening and diagnostic mammograms are initially the same exams. Screening mammograms may be done with 2D or 3D technique. 3D technique may decrease the need to return for additional imaging since the breast is viewed as "slices" rather than as overlapping structures. It may also for the same reason allow earlier detection of an abnormality, but there is a tradeoff in increased radiation dose.
Diagnostic Mammograms
A diagnostic exam may be 2D or 3D and is checked by a radiologist while the patient is on site and additional views are obtained only if needed. Diagnostic mammograms are done for women experiencing or displaying symptoms that could be linked to breast cancer, such as nipple discharge or unusual lumps. Diagnostic mammograms may be more involved than a screening exam and entail the creation of several specialized images from various angles. Diagnostic imaging is used to confirm any abnormalities found during a screening mammogram or self-examination. Ultrasound evaluation is frequently performed in conjunction with a diagnostic mammogram to add to specificity and sensitivity.
"Call back" mammograms are special diagnostic images obtained as a followup to an abnormal screening exam. Again, ultrasound is frequently performed at the time of a call back exam.
What is the Mammogram X-ray Process?
The mammogram process is relatively simple, straightforward, and noninvasive. The entire process takes no more than 30 minutes from beginning to end and has no recovery period.
Discomfort is limited to breast compression, which is necessary to reduce the amount of radiation emitted during the procedure and to reduce overlapping shadows which may obscure an abnormality. Breast compression is key to optimal mammography: the more compression one allows, the better the images.
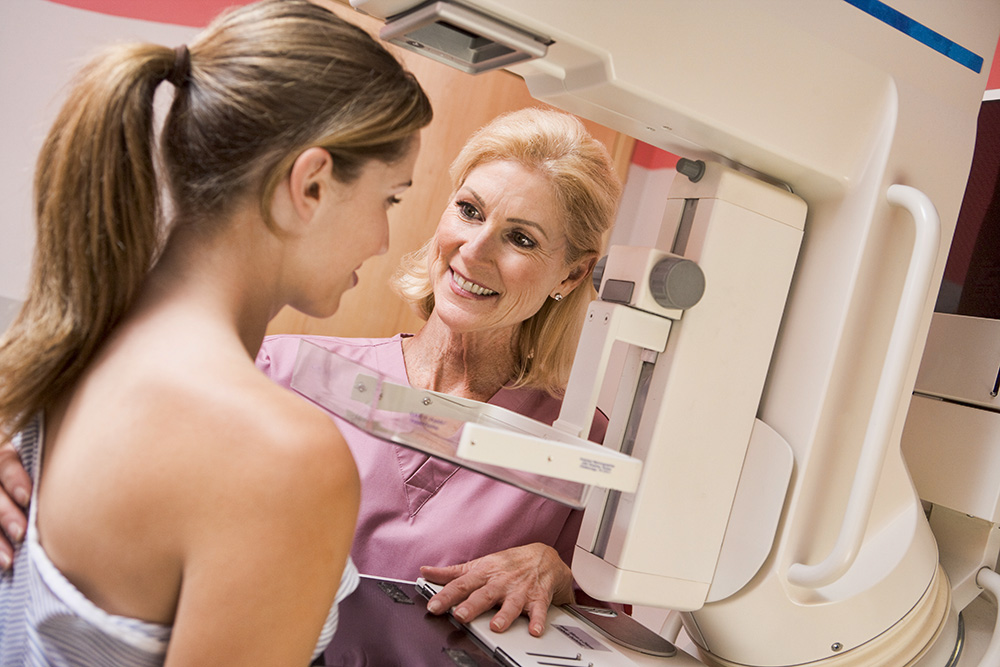
The first step of a mammogram procedure is to change into a medical gown. Typically women will be asked to remove their clothing from the waist up.
Next, a technician will ask the patient if they have noticed any unusual lumps, bumps, or unusual moles. A marking tape will be placed on the areas indicated. Markers may also be placed on existing benign moles or scars that may interfere with the imaging procedure and interpretation of the data.
Breast Cancer Symptoms
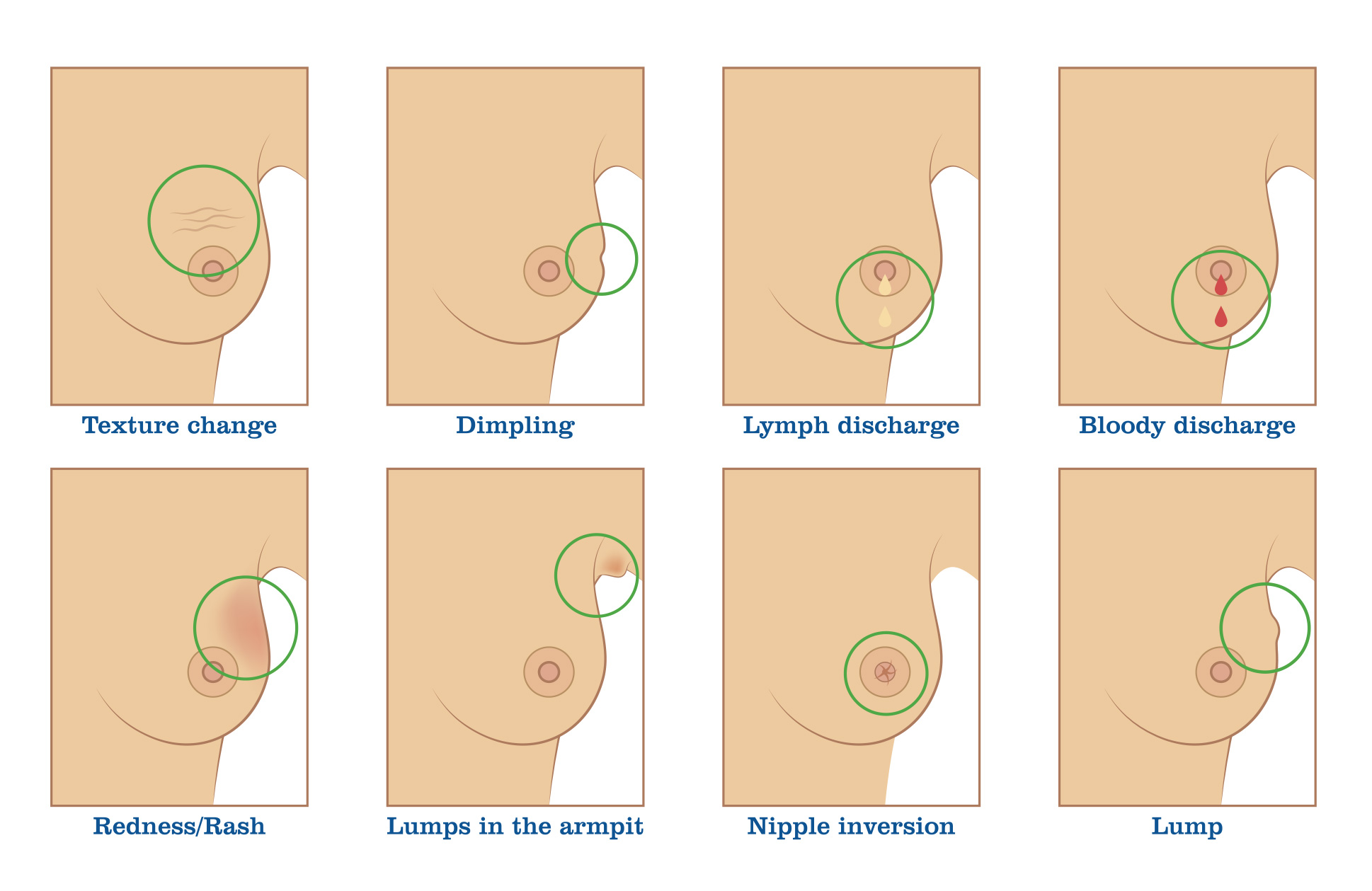
Once markers have been placed, the patient will stand in front of the mammogram machine. One breast at a time is placed on the imaging plate and compressed by another plastic plate to optimize visualization of the soft tissues.
The patient is then asked to take a deep breath and then hold it to reduce movement while images are taken.
Once images have been obtained the patient can change from the medical gown into their original clothing. Images are then processed and interpreted by a radiologist.
What Are the Risks of Mammograms?
While mammograms are critical for the early detection and successful treatment of breast cancer in women, they are not entirely without risks.
While mammograms do rely on radiation in the form of x-rays to produce images, the risks associated with the amount of radiation are outweighed by the benefits.
In order to detect cancer early, radiologists must report any suspicious finding, therefore not all abnormalities are cancer, resulting in false positive exams, exams that are initially thought to be abnormal, but prove not to be. Patients' understanding that needing to return for additional images is necessary to detect the most cancers early and inherent to the screening process is important.
How Much Do Mammograms Cost?
Screening mammograms are covered by most health insurance plans. Depending on a patient’s plan, patients may pay nothing at all or a small co-pay. The out-of-pocket, or cash price ranges from $100 to $300 with most facilities able to offer screenings on the lower end of that range. Green Imaging offers affordable self-pay mammograms starting as low as $125.
Diagnostic mammograms typically cost more ($175 unilateral, $200 bilateral at Green Imaging) and will fall in the higher end of that range. Costs will vary from one facility or diagnostic imaging provider to the next and from one facility to the next. A diagnostic mammogram obtained at a large hospital will often cost more than one done at an imaging facility or clinic somewhere else.
Prior Exams
Availability of prior mammographic exams adds to the sensitivity of the exam. Returning to the same facility or providing prior studies obtained elsewhere to the current facility in advance of the exam may preclude the need to return for additional images and shortens the reporting interval.
The Green Imaging Difference
At you can save between 50 and 80% of your out-of-pocket costs for MRI, CT, ultrasounds, and other high-quality imaging services. Affordable self-pay mammograms start as low as $125, compared with $300 at other imaging facilities in the Houston and other metropolitan areas in Texas.
Don’t pay secret rates for a Mammogram. Go Green Imaging instead!